หมอนรองกระดูกปลิ้นกดทับเส้นประสาท โรคยอดฮิตที่รักษาได้ และไม่น่ากลัวอย่างที่คิด

หมอนรองกระดูกปลิ้นกดทับเส้นประสาท เป็นอาการที่พบได้บ่อยในกลุ่มผู้ที่มีอาการปวดหลังร้าวลงขา เพราะกระดูกสันหลังบริเวณนี้รับน้ำหนักมาก และมีการเคลื่อนไหวค่อนข้างเยอะกว่ากระดูกสันหลังส่วนอื่นๆ ทำให้หมอนรองกระดูกอาจจะเกิดการแตกปลิ้นออกมาจนกดเบียดเส้นประสาท โดยจะมีอาการปวดหลังช่วงเอวต่อกับสะโพก ร่วมกับปวดร้าวลงขา ซึ่งส่วนใหญ่แล้วมักจะเป็นที่ขาข้างใดข้างหนึ่ง อาจมีอาการชาหรืออ่อนแรงร่วมของขาหรือปลายเท้าร่วมด้วยได้
มักพบในผู้ป่วยอายุระหว่าง 20-50 ปี โดยปัจจัยเสี่ยงที่ทำให้เกิดโรคนี้คือการทำงานที่ต้องยกของหนัก น้ำหนักตัวมาก การสูบบุหรี่ การบิดตัวหรือก้มหลังอย่างรวดเร็วและรุนแรง เป็นต้น
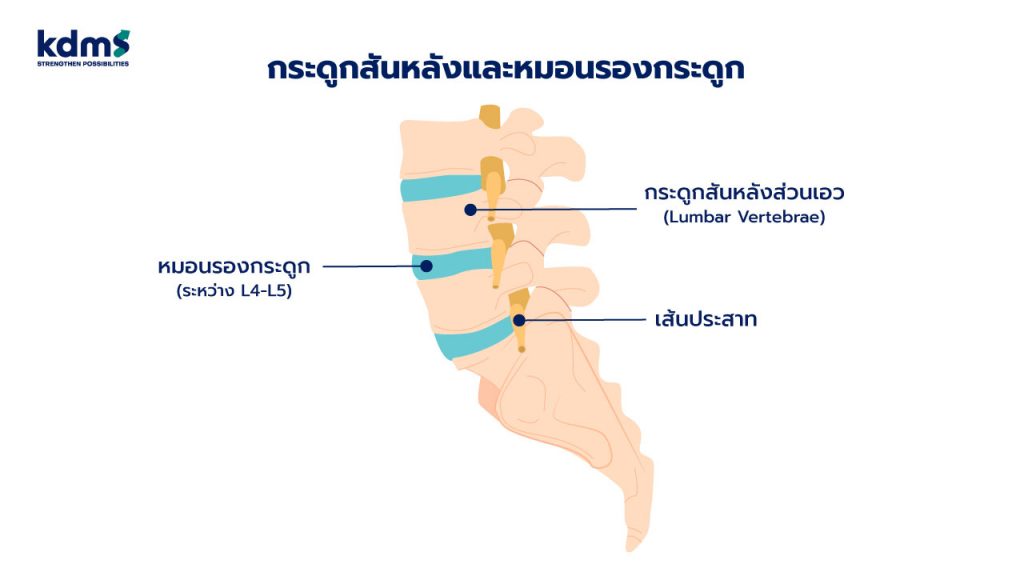
Table of Contents
ทำความรู้จักหมอนรองกระดูก มันคือส่วนไหนในร่างกาย และทำหน้าที่อะไร
แนวกระดูกสันหลังของคนเราจะประกอบไปด้วยตัวกระดูก และมีหมอนรองกระดูกที่คั่นอยู่ในแต่ละชั้น โดยหน้าที่ของหมอนรองกระดูกคือช่วยในการรับน้ำหนักของร่างกาย เหมือนเป็นตัวประคองระหว่างชั้นของกระดูกสันหลังเพื่อให้สามารถเคลื่อนไหวได้อย่างยืดหยุ่น
แม้จะมีชื่อว่าหมอนรองกระดูก แต่จริงๆ แล้วโครงสร้างส่วนใหญ่ของมันประกอบด้วยน้ำ คอลลาเจน และส่วนประกอบอื่นๆ เช่น โปรตีน ซึ่งหากดูตามภาพจะเห็นว่าโครงสร้างภายในจะประกอบด้วย 2 ส่วนหลักๆ ได้แก่
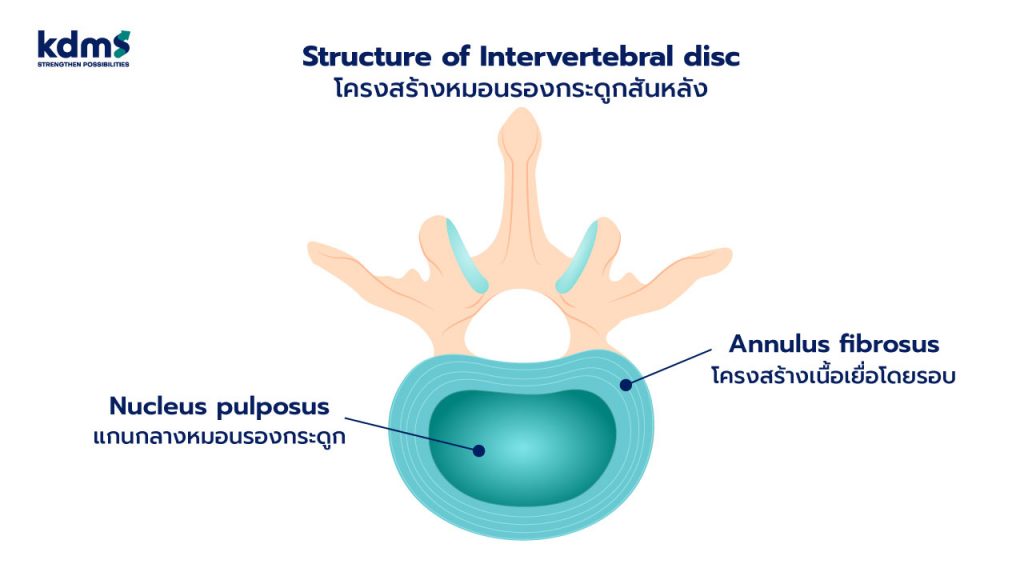
1. Nucleus pulposus
Nucleus pulposus คือแกนกลางหมอนรองกระดูก โดยมีส่วนประกอบหลักเป็นคอลลาเจนกับน้ำที่มากถึง 80% ทำหน้าที่รับแรงกระแทก และช่วยกระจายแรงของนํ้าหนักตัวที่ส่งผ่านมายังกระดูกสันหลังแต่ละข้อในขณะที่เคลื่อนไหวร่างกาย
2. Annulus fibrosus
Annulus fibrosus คือโครงสร้างเนื้อเยื่อโดยรอบที่คอยห่อหุ้ม Nucleus pulposus ด้านในไม่ให้ปลิ้นออกมา มีหน้าที่ทำให้ข้อต่อระหว่างกระดูกสันหลังมีความมั่นคงแข็งแรง สามารถรับแรงในแนวบิด หมุน เอียง หรือก้มเงยได้ดี
นอกเหนือจากเรื่องลักษณะโครงสร้างแล้ว ความพิเศษอย่างหนึ่งของหมอนรองกระดูกคือมันเป็นส่วนประกอบของร่างกายที่ไม่มีเลือดเข้าไปหล่อเลี้ยงโดยตรงเพื่อแลกเปลี่ยนสารอาหาร ออกซิเจน และของเสีย แต่จะใช้แรงดันของกระดูกที่กดมาที่ตัวหมอนรองกระดูกขณะที่เราเคลื่อนไหวร่างกายในการแลกเปลี่ยนสารอาหารระหว่างกัน ส่งผลให้กระบวนการซ่อมแซมตัวเองของมันไม่ค่อยดีนัก จึงเป็นเหตุผลว่าเมื่อใดก็ตามร่างกายของเรามีอาการหมอนรองกระดูกปลิ้น นั่นหมายความว่ามันอาจเป็นจุดเริ่มต้นความเสื่อมของกระดูกสันหลังแบบหนึ่ง
สาเหตุของหมอนรองกระดูกปลิ้นกดทับเส้นประสาท
อย่างที่อธิบายไปแล้วว่าหมอนรองกระดูกทำหน้าที่ในประคองและกระจายแรงในการรับน้ำหนักของกระดูกสันหลังโดยตรง เพราะฉะนั้นปัจจัยเสี่ยงหลักๆ จะเน้นไปในเรื่องการรับน้ำหนักและความเคลื่อนไหวที่รุนแรงและรวดเร็ว ซึ่งจะเป็นการเพิ่มโอกาสให้หมอนรองกระดูกแตกปลิ้นออกมา ดังนี้
1. น้ำหนักตัวมาก
เพราะยิ่งน้ำหนักตัวมาก กระดูกสันหลังก็ต้องรับน้ำหนักมากตามไปด้วย
2. การใช้งานที่ไม่เหมาะสม
เช่น ก้มหลัง ยกของหนัก เพราะท่าทางเหล่านี้เป็นการเพิ่มแรงดันที่หมอนรองกระดูกค่อนข้างเยอะ ซึ่งอาจจะเกินความทนทานที่หมอนรองกระดูกรับได้ จนกระทั่งเกิดการแตกปลิ้นออกมา
3. การนั่งในท่าที่ไม่เหมาะสมต่อเนื่องเป็นเวลานานๆ
พบมากในกลุ่มคนวัยทำงาน และมักจะมีโอกาสเกิดหมอนรองกระดูกปลิ้นกดทับเส้นประสาทในบริเวณช่วงเอวมากที่สุด เพราะเวลาที่นั่งนานๆ กระดูกสันหลังส่วนนั้นจะรับน้ำหนักแบบเต็มๆ
4. การไอหรือจามแรงๆ
เป็นสาเหตุหนึ่งของการเพิ่มแรงดันอย่างฉับพลันในหมอนรองกระดูก
5. คนที่สูบบุหรี่จัด
บุหรี่จะทำให้หมอนรองกระดูกสันหลังเสื่อมก่อนวัยอันควร และทำให้หมอนรองกระดูกเกิดการแตกปลิ้นได้มากขึ้น

การเกิดหมอนรองกระดูกปลิ้นกดทับเส้นประสาทมี 3 รูปแบบ
1. Protusion
ตัวนิวเคลียสด้านในมีการทะลักออกมา โดยที่ขอบด้านนอกยังไม่เกิดการฉีกขาด
2. Extrusion
ขอบด้านนอกมีการขาดออก และมีนิวเคลียสทะลักออกมาโดยที่ยังติดกับด้านในอยู่ ไม่ได้หลุดออกมาเป็นชิ้นอิสระ
3. Sequestration
ขอบด้านนอกมีการขาดออก โดยที่นิวเคลียสมีการปลิ้นหลุดออกมาเป็นชิ้นอิสระจากด้านใน
อาการปวดในช่วงแรกจะค่อนข้างมาก ซึ่งเกิดขึ้นจาก 2 ปัจจัยคือ ปริมาณการกดทับของเส้นประสาท และการอักเสบจากการแตกปลิ้นของหมอนรองกระดูก คนไข้ประมาณ 80% ที่ทำการรักษาอาการจะค่อยๆ ดีขึ้นใน4-6 สัปดาห์ แต่จะมีส่วนที่เหลือที่อาการอาจจะไม่ดีขึ้น เนื่องจากมีหมอนรองกระดูกกดทับเส้นประสาทมาก ซึ่งอาจจะต้องรักษาโดยการผ่าตัด
เมื่อเป็นโรคหมอนรองกระดูกปลิ้นกดทับเส้นประสาท ทำไมถึงรู้สึกปวดร้าวลงขาเพียงข้างเดียว
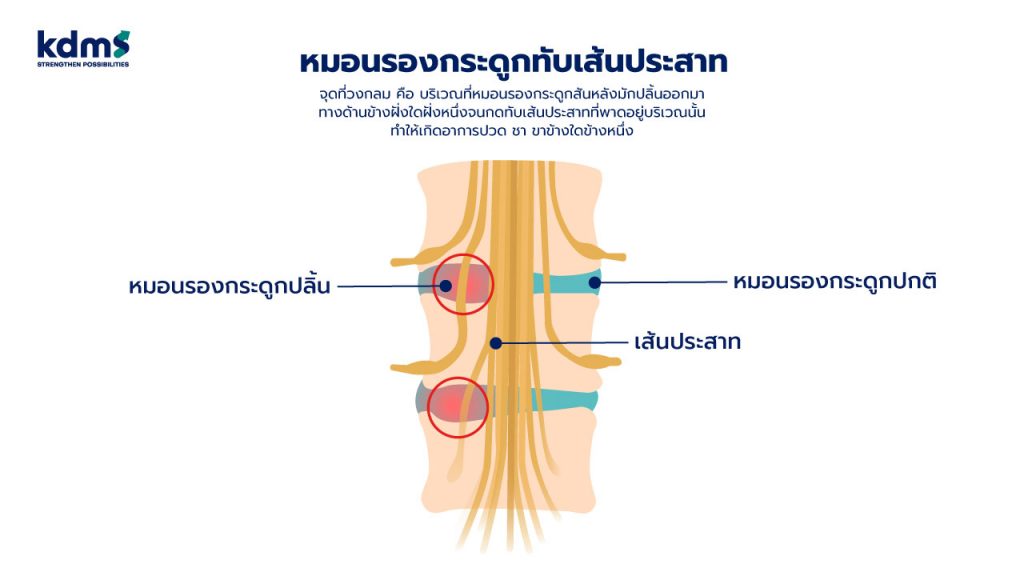
หากดูตามภาพประกอบ จุดที่วงกลมในภาพจะเป็นบริเวณที่หมอนรองกระดูกสันหลังมักจะปลิ้นออกมาทางด้านข้างฝั่งใดฝั่งหนึ่งมากกว่าที่จะปลิ้นออกมาตรงกลาง ซึ่งบริเวณนี้จะมีเส้นประสาทพาดผ่านอยู่ ทำให้ผู้ป่วยที่เป็นโรคหมอนรองกระดูกปลิ้นกดทับเส้นประสาทส่วนใหญ่จะมีอาการปวดร้าวชาลงขาเพียงข้างใดข้างหนึ่ง
ขั้นตอนการวินิจฉัยโรคหมอนรองกระดูกปลิ้นกดทับเส้นประสาท
โดยปกติแพทย์จะเริ่มต้นจากการซักประวัติและตรวจร่างกายก่อน ซึ่งเฉพาะสองขั้นตอนนี้ก็สามารถวินิจฉัยโรคได้เบื้องต้นแล้วว่าผู้ป่วยเป็นโรคหมอนรองกระดูกปลิ้นกดทับเส้นประสาทหรือไม่
แต่เพื่อความชัดเจนมากยิ่งขึ้น แพทย์จะทำการตรวจร่างกายด้วยเครื่องถ่ายภาพด้วยคลื่นแม่เหล็กไฟฟ้า หรือ MRI (Magnetic Resonance Imaging) เพื่อให้ได้ผลยืนยันออกมาชัดเจนร้อยเปอร์เซ็นต์ เพราะการทำ MRI จะเห็นโครงสร้างของหมอนรองกระดูกสันหลังและเส้นประสาทได้ชัดเจน ทำให้สามารถบอกได้ว่ามีการกดทับเส้นประสาทที่ตำแหน่งใดมากน้อยแค่ไหน เพื่อวางแผนการรักษาต่อไป
แนวทางการรักษาโรคหมอนรองกระดูกปลิ้นกดทับเส้นประสาท
1. รักษาด้วยการใช้ยา
การรักษาด้วยการใช้ยาจะเป็นการจ่ายยาตามโรคของผู้ป่วย เช่น ยาแก้ปวด, ยาลดการอักเสบ, ยาคลายกล้ามเนื้อ หรือยาลดความปวดของระบบประสาท เป็นต้น
นอกจากยารับประทานแล้วก็ยังมีทางเลือกหนึ่งคือการฉีดยาระงับปวดลดอาการอักเสบที่เส้นประสาท วิธีนี้แพทย์จะให้ผู้ป่วยทำ MRI เพื่อหาตำแหน่งที่หมอนรองกระดูกปลิ้นกดทับเส้นประสาทอยู่ จากนั้นจะฉีดยาเข้าไปในบริเวณใกล้กับเส้นประสาทที่โดนหมอนรองกระดูกกดทับ โดยใช้เครื่อง X-Ray เป็นตัวบอกตำแหน่ง เพื่อลดอาการปวดและอักเสบของเส้นประสาท
2. รักษาโดยไม่ใช้ยา
กายภาพบำบัด
การกายภาพบำบัด เช่น การนวด อัลตราซาวด์ การใช้เลเซอร์ รวมไปถึงการทำช็อกเวฟเพื่อคลายกล้ามเนื้อ ลดอาการปวด นอกจากนี้ยังมีท่ากายบริหารยืดเหยียดและเสริมสร้างความแข็งแรงให้กล้ามเนื้อ
การปรับเปลี่ยนพฤติกรรมของผู้ป่วย
แพทย์จะวิเคราะห์จากการซักประวัติว่าผู้ป่วยมีพฤติกรรมที่ไม่ถูกต้องอย่างไรบ้าง และควรแก้ไขอย่างไร
3. รักษาด้วยการผ่าตัด
วิธีนี้จะเกิดขึ้นในกรณีของผู้ป่วยที่ผ่านการรักษาในสองรูปแบบข้างต้นมาแล้วอาการปวดยังไม่ดีขึ้น ซึ่งรูปแบบการผ่าตัดสำหรับโรคหมอนรองกระดูกปลิ้นกดทับเส้นประสาท จะมีดังต่อไปนี้
1. การผ่าตัดหมอนรองกระดูกแบบเปิดแผล (Open discectomy)
เป็นวิธีการผ่าตัดแบบเริ่มแรกตั้งแต่สมัยก่อน โดยจะเป็นการเปิดแผลในบริเวณที่หมอนรองกระดูกถูกกดทับในความกว้างประมาณ 7-8 เซนติเมตร เพื่อที่จะนำหมอนรองกระดูกที่ถูกกดทับอยู่ออกไป
2. การผ่าตัดโดยหมอนรองกระดูกโดยใช้กล้องกำลังขยายสูง (Microscopic discectomy)
วิธีนี้จะช่วยให้แผลผ่าตัดเล็กลงเหลือเพียง 2-3 เซนติเมตร โดยแพทย์จะมีตัวช่วยเป็นกล้อง Microscope ที่มีกำลังขยายมากกว่าปกติ 20-100 เท่า ซึ่งจะทำให้เห็นรายละเอียดของเส้นประสาทอย่างชัดเจนมาก โดยไม่จำเป็นเปิดแผลกว้างเหมือนการผ่าตัดแบบปกติ
3. การผ่าตัดหมอนรองกระดูกผ่านกล้อง Endoscope (Endoscopic discectomy)
การผ่าตัดหมอนรองกระดูกผ่านกล้อง Endoscope เป็นการผ่าตัดกระดูกสันหลังผ่านกล้อง Endoscope โดยแพทย์จะทำการเจาะรูสอดท่อขนาดเล็ก และสอดอุปกรณ์เข้าไปเพื่อทำการผ่าตัดหมอนรองกระดูกออกมา ซึ่งวิธีนี้จะทำให้แผลจากการผ่าตัดมีขนาดเล็กมากเพียง 8 มิลลิเมตรเท่านั้น
การพัฒนาวิธีการผ่าตัดที่ทำให้แผลเล็กลงนั้น นอกจากแผลที่เราเห็นจากภายนอกจะเล็กลงแล้ว ข้อดีอื่นๆ ที่สำคัญกว่าขนาดแผลคือ กล้ามเนื้อหลัง กระดูกสันหลังส่วนที่ดีอยู่ก็จะบาดเจ็บจากการผ่าตัดลดลง ทำให้เสียเลือดน้อยลง ความเจ็บหลังผ่าตัดน้อยกว่าวิธีปกติ กลับมาลุกยืนเดินได้ทันทีหลังผ่าตัดในวันแรก ทำให้เวลาที่ใช้ในการฟื้นฟูสภาพร่างกายหลังผ่าตัดน้อยลง ทำให้ผู้ป่วยสามารถกลับไปทำงานและใช้ชีวิตประจำวันได้อย่างรวดเร็ว
กล่าวโดยสรุปคือ โรคหมอนรองกระดูกปลิ้นกดทับเส้นประสาทนั้น อาจพูดได้ว่าปัจจัยเสี่ยงส่วนใหญ่เกิดมาจากพฤติกรรมการใช้งานแทบทั้งสิ้น เพราะฉะนั้นหนทางป้องกันที่ดีที่สุดคือการเริ่มต้นปรับเปลี่ยนพฤติกรรมตั้งแต่วันนี้ เพราะเพียงการเปลี่ยนแปลงเล็กๆ ก็สามารถช่วยแบ่งเบาภาระกระดูกสันหลังของเราได้แล้ว
Q&A
Q: หลังการผ่าตัดรักษาโรคหมอนรองกระดูกปลิ้นกดทับเส้นประสาท ต้องใช้เวลาพักฟื้นนานแค่ไหน
หลังจากผู้ป่วยทำการผ่าตัดเรียบร้อยแล้ว อาการปวดร้าวลงขาจะดีขึ้นทันที ส่วนอาการชาหรืออ่อนแรงจะค่อยๆ ดีขึ้นตามลำดับ
2 สัปดาห์หลังผ่าตัด ผู้ป่วยจะเริ่มกลับไปทำกิจกรรมเบาๆ ได้ เช่น นั่งทำงาน ขับรถ เดินยืนระยะไกลๆ ได้ แต่ยังต้องหลีกเลี่ยงการยกของหนักหรือการก้มเงยหลังมากๆ ไปก่อน ส่วนการใช้งานแบบเต็มรูปแบบ ทั้งการทำงานปกติและออกกำลังกาย จะสามารถทำได้ภายใน 6-8 สัปดาห์
Q: เคยเป็นโรคหมอนรองกระดูกปลิ้นกดทับเส้นประสาทมาแล้ว จะมีโอกาสเป็นซ้ำได้อีกไหม
จากการศึกษาพบว่ามีโอกาสเป็นซ้ำได้อีกหลังผ่าตัด 10-15% ทั้งนี้ เราสามารถลดความเสี่ยงของโอกาสที่จะเป็นซ้ำได้ด้วยการปรับพฤติกรรมการใช้งานหลังที่ไม่ถูกวิธี ไม่ว่าจะเป็นการก้มหลัง ยกของหนักๆ การสูบบุหรี่ และต้องพยายามควบคุมน้ำหนักไม่ให้มากจนเกินไป เพื่อลดแรงดันที่จะเกิดขึ้นกับหมอนรองกระดูก
Q: ทำไมการนั่งหลังค่อมหรือก้มหลังยกของจึงส่งผลเสียต่อหมอนรองกระดูก?
จริงๆ แล้วในทุกๆ การเคลื่อนไหว ไม่ว่าจะนั่ง เดิน ยืน หรือนอน กระดูกสันหลังที่เป็นแกนกลางของร่างกายกำลังทำหน้าที่รับน้ำหนักของเราอยู่ตลอดเวลา นั่นหมายความว่าถ้าเราทำกิจวัตรประจำวันในท่าทางที่ไม่ถูกต้อง กระดูกสันหลังก็จะทำงานมากขึ้น จนอาจก่อให้เกิดอาการปวดหลังตามมา
เคยมีผลการศึกษาออกมาแล้วว่าท่าทางต่างๆ ในชีวิตประจำวันของเราส่งผลต่อการรับน้ำหนักของกระดูกสันหลังแตกต่างกันอย่างไรบ้าง ซึ่งพบว่าหากเรายืนหลังตรงปกติ กระดูกสันหลังจะรับน้ำหนักเต็มๆ ที่ 100% อยู่แล้ว แต่หากอยู่ในท่านั่ง กระดูกสันหลังจะรับน้ำหนักมากขึ้นไปอีกที่ 140-185% นั่นเป็นเพราะน้ำหนักทั้งตัวไม่ได้ถูกแบ่งเบาไปที่ร่างกายท่อนล่าง แต่มากองรวมกันอยู่ที่ช่วงเอว ยิ่งถ้านั่งพร้อมกับยกของไปด้วย การรับน้ำหนักจะทวีคูณขึ้นไปที่ 275% เลยทีเดียว เมื่อกระดูกสันหลังรับน้ำหนักมาก แน่นอนว่าหมอนรองกระดูกต้องได้รับผลกระทบไปด้วยเช่นกัน
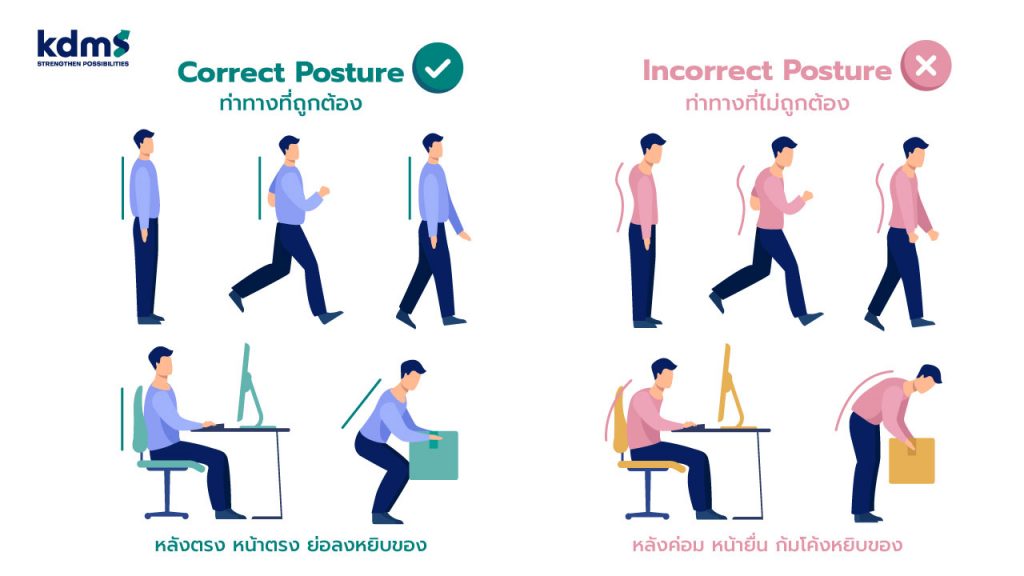
ฉะนั้นท่าทางที่ถูกต้องในการที่จะช่วยลดภาระให้การรับน้ำหนักของกระดูกสันหลัง คือการยืน เดิน นั่ง โดยพยายามให้หลังอยู่ในแนวตรงอยู่เสมอ หลีกเลี่ยงการยกของหนักโดยไม่จำเป็น เพื่อเป็นการลดแรงดันที่จะเกิดกับหมอนรองกระดูกของเรานั่นเอง


 history
history